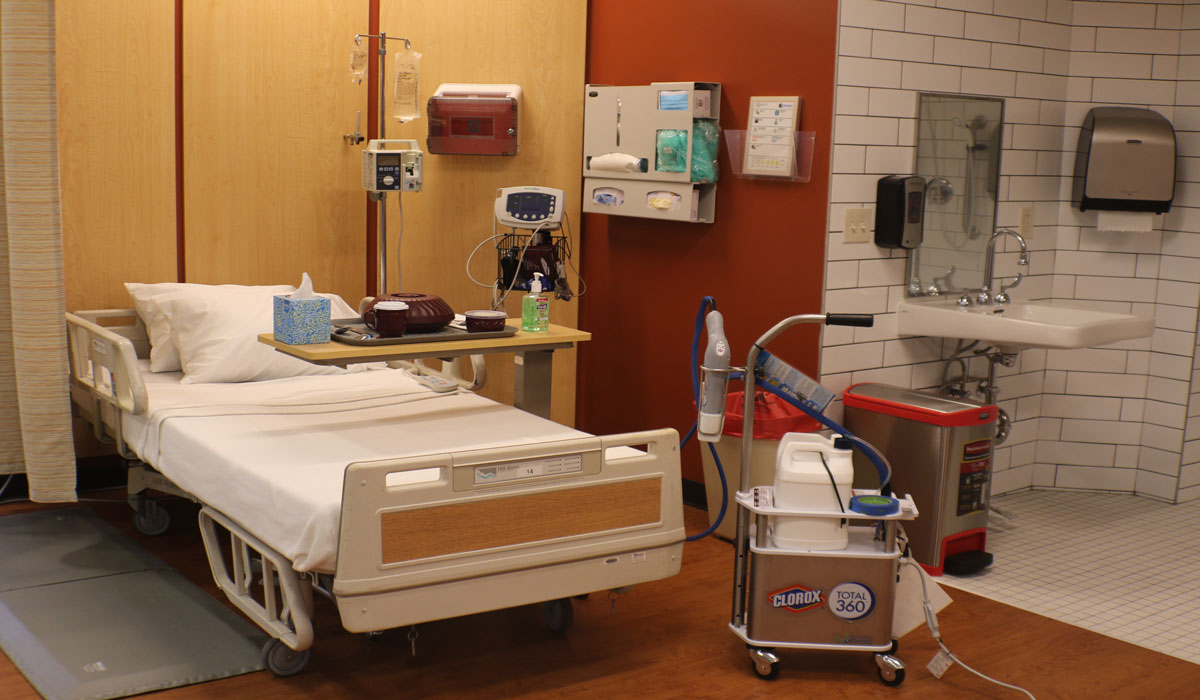
Unclean Hospital Rooms and Patient Risk
Hospitals are under intense pressure to be economically efficient, which most often translates to cutting staff and costs. Often, one of the first areas to be cut is in the resources for infection control and cleaning, generally handled by the Environmental Services (ES) team.
Research Study
A study by the Ontario Council of Hospital Unions (OCHU) and the Canadian Union of Public Employees linked cuts to cleaning staff to a rise in hospital-acquired infections. These hospital-acquired infections include bacteria such as MRSA, C. Difficile, and VRE, all of which have become more common in recent years.
Another study by the Society for Healthcare Epidemiology of America (SHEA), examined hospital rooms worldwide to measure the effectiveness of hospital environmental cleaning procedures. Specifically, samples were taken from hospital rooms and nursing stations, and it was found that some multidrug-resistant organisms (MDROs) were able to survive. The study concluded that, “More frequent and better cleaning [is] needed to remove biofilms and MDROs from hospital surfaces and the environment.”
Given this data, and the rise in hospital-acquired infection deaths, some groups are drawing a relationship between hospital underfunding and a rise in preventable deaths. Rather than cutting hospital cleaning staff and procedures, facilities should be enabling a high-quality environmental services team, a key component for maintaining cleanliness and avoiding outbreaks.
Understanding the problem
To tackle this problem, researchers at Johns Hopkins are exploring ways to improve patient room cleaning with a three-year study aimed at developing solutions to make the hospital environment safer. The group is examining the work systems, tools, and technologies the ES team deploys in cleaning and disinfecting patient care areas in order to, “understand what some of the barriers and challenges to patient room cleaning tasks are, what strategies environmental services associates have developed to get rooms cleaned in a timely manner, and what ideas various stakeholders have for improvement,” says Ayse P. Gurses, Ph.D., M.P.H., Associate Professor of Anesthesiology and Critical Care Medicine at the Johns Hopkins University School of Medicine.
It is likely that this, and other studies, will highlight the importance of a fully staffed and properly trained environmental services team in maintaining low hospital-acquired infection rates. Additional studies looking at cleaning products and methods are also underway. However, one thing is clear: cleaning and disinfecting should be a top priority of any healthcare facility.
While further investigation is needed, it seems intuitive that investing in cleanliness up front is much less expensive than caring for patients in the intensive care unit who have a healthcare acquired infection. All aspects of cleanliness, from time-spent, to processes, to products used, should be examined to ensure a safer healthcare environment for workers and for patients.
About Johnston
Johnston has always stood for reliability, commitment, quality, and service. Our heritage means years of accumulated industry knowledge, the ability to see the bigger picture, and the know-how to determine the best possible approach. Combining this mastery with the drive to deliver exceptional results, Johnston goes beyond sales, developing strategic, end-to-end tailored solutions for each customer since 1881.